Human papillomavirus-associated oropharyngeal squamous cell carcinoma (HPVOPSCC) accounts for approximately 85 percent of all oropharyngeal cancers nationwide. As the incidence continues to rise, Mount Sinai researcher Raymond Chai, MD, FACS, is concerned about the impacts of the standard of care among patients who present with this disease.
“We are applying the same therapeutic modality as we do for environmentally related oropharyngeal squamous cell carcinoma from smoking and alcohol consumption, which is lots of chemotherapy and lots of radiation,” says Dr. Chai, Associate Professor, Otolaryngology (Head and Neck Surgical Oncology), Institute for Thyroid, Head, and Neck Cancer at the Icahn School of Medicine at Mount Sinai.
Despite excellent cure rates, these therapies often result in negative side effects, including dry mouth, hearing loss, neuropathy, muscle fibrosis, and difficulty in swallowing. Rarer but potentially life-altering late complications can include cranial nerve deficits and necrosis of the jaw. Many of these patients, who are young and healthy, must live with the lifelong side effects of this toxic treatment. It is a problem Dr. Chai aims to solve through an innovative study: the Sinai Robotic Surgery Trial in HPV-Positive Oropharyngeal Squamous Cell Carcinoma (SIRS 2.0). The study is assessing the potential of achieving cancer control and survival rates that are comparable to the standard of care through transoral robotic surgery (TORS) alone or in combination with greatly reduced doses of radiation and chemotherapy among patients with HPVOPSCC.
“We are investigating how we can greatly de-intensify therapy to improve our patients’ long-term quality of life without impacting the outcomes we are seeing,” Dr. Chai says.
Testing for Circulating HPV Tumor DNA in the Blood
The trial builds on the findings of the earlier SIRS 1.0 study, a non-randomized phase 2 study in which patients with early stage HPVOPSCC who underwent TORS followed by reduced-dose radiation demonstrated highly favorable survival rates with excellent function. What makes this trial unique is that Dr. Chai is using NavDx®, a test that measures circulating HPV tumor DNA in the blood. The test offers a biomarker to predict treatment response and likelihood of cancer recurrence among patients with HPVOPSCC, and thus potentially enable either complete avoidance or significant de-escalation of adjuvant chemoradiotherapy. Data from existing studies suggest that HPV circulating tumor DNA (ctDNA) during the surveillance period following treatment is a highly accurate test for the detection of microscopic residual disease.
“Traditionally, the decision as to whether to administer radiation or chemotherapy following surgery was based on predicted risk level for recurrence from the pathology results, but there is no strong data informing that decision,” Dr. Chai says. “However, many of these patients receiving these treatments likely would do equally well if they did not undergo radiation or chemo. We just do not know who they are. This is one of the first studies in the world to use HPV ctDNA, which detects microscopic levels of residual disease in the blood, to identify those patients. Based on the results we see, this test has the potential to be an effective new paradigm for treatment.”
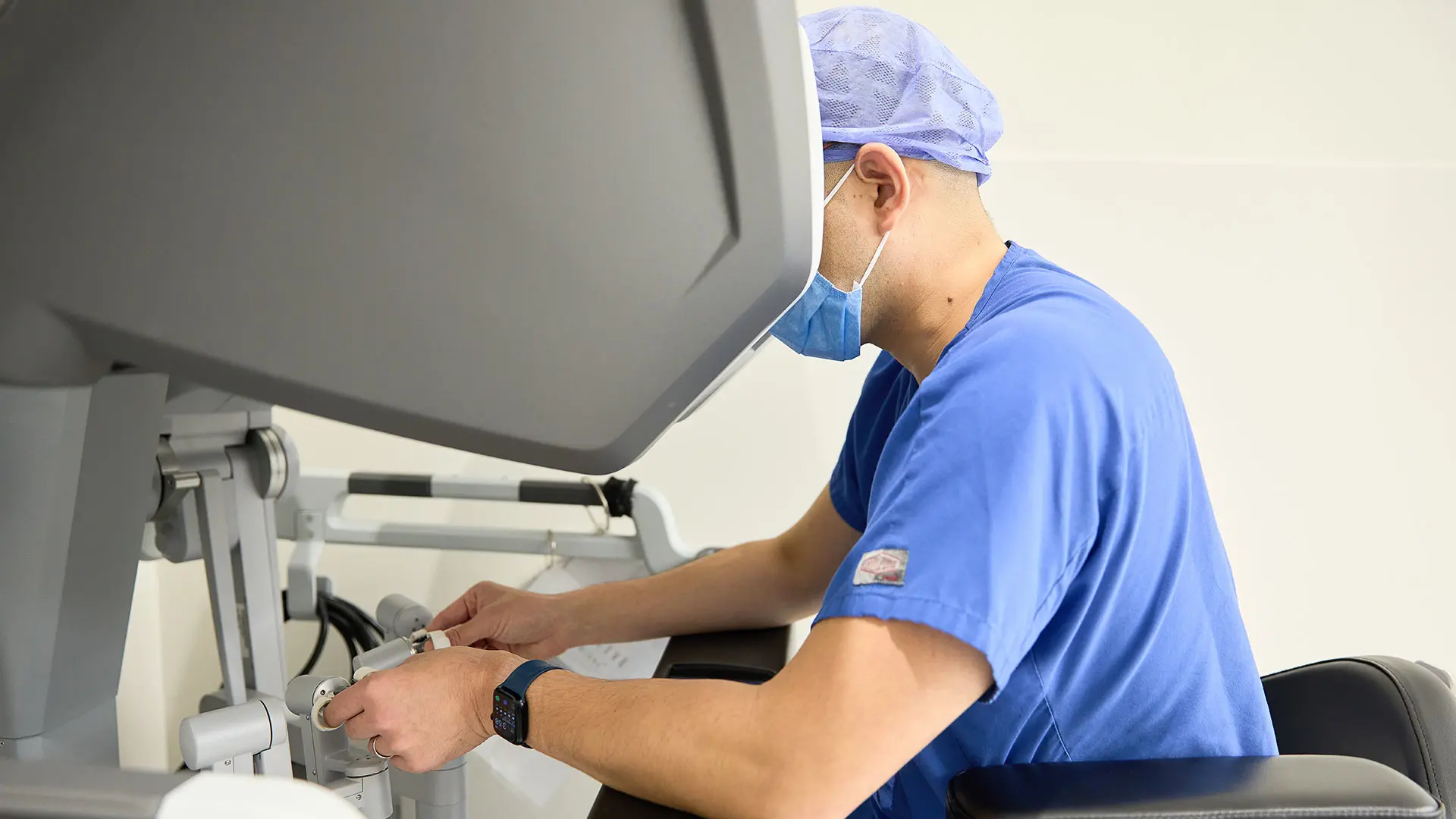
Raymond Chai, MD, FACS, performing TORS.

Close-up of Dr. Chai performing TORS.
How the Trial Will Be Performed
The trial will recruit 200 individuals who have been diagnosed with HPVOPSCC, have a positive preoperative HPV ctDNA test, and who have not received any prior chemotherapy, radiation therapy, or surgery for their cancer. All participants must demonstrate overexpression of p16 (a known surrogate for HPV-mediated disease) and positive HPV DNA expression on a polymerase chain reaction test. Patients with a history of more than 20 years of smoking, or who are active smokers, are excluded from the trial.
Mount Sinai researchers will be looking at recurrence rates within the first two years of surgery among two groups of patients with early stage HPVOPSCC and undetectable HPV ctDNA: those with early stage disease who are treated with surgery alone (low-risk group) and those who are treated with surgery and a significantly de-intensified adjuvant chemoradiotherapy protocol of 46 Gy, with Gy being the unit of measurement for the radiation dose that patients receive (high-risk group). The research team will also collect blood and tumor samples from participants to gain more insights into the biological factors that influence the growth and response of HPVOPSCC to treatment. Furthermore, patients will participate in quality-of-life surveys to gain additional insights on outcomes.
Although this trial is exploratory and further studies are warranted, Dr. Chai believes the results could be a game-changer for patients with HPVOPSCC. “We believe this therapeutic approach has the potential not just to decrease the toxicity necessary to maintain the outstanding cure rates we are able to achieve, but also to streamline the logistical requirements of treatment—the time off work, the constant travel—that have significant impacts on patients’ lives,” he says.
Featured

Raymond Chai, MD, FACS
Associate Professor, Otolaryngology – Head and Neck Surgical Oncology
